Introduction
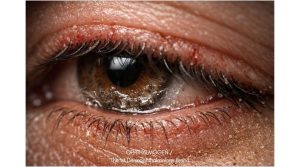
The eye is not an isolated organ. It is surrounded and supported by a set of structures – eyelids, eyelashes, eyebrows, and periorbital skin – that work together as a single system.
This “whole” is called OPHTHALMODERMA.
The Dermophthalmology introduces this new concept to describe the ecosystem that connects health, comfort, beauty, and vision.
Embryological Origin: A Shared Ectodermal Tissue
The eye and the skin share a common embryological origin::
- Τhe ectoderm gives rise to both the ocular surface (corneal epithelium, conjunctiva) and the skin.
- Οι Eyelashes and eyebrows develop from the same layers that form skin and hair.
This explains why many dermatological diseases also manifest in the eyes.
Components of the Ophthalmoderma

The Ophthalmoderma includes::
- Eyelids: protection, tear film distribution, blinking mechanism.
- Eyelashes: defense against dust and microbes; micro-ecosystem with Demodex and bacteria.
- Eyebrows: barrier against sweat and sebum; contribution to expression.
- Periorbital skin: thinner, more vulnerable to aging.
- Ocular surface: tear film, cornea, conjunctiva; key for comfort and quality of vision.
All these elements are interconnected. A disturbance in one (e.g., blepharitis) affects the entire system..
Pathologies Highlighting the Unity

- Rosacea: simultaneous involvement of skin and eyelids.
- Seborrheic dermatitis: dandruff on eyelashes + eyelid irritation.
- Psoriasis: lesions on skin and eyelids.
- Dyskeratoses: dryness and desquamation impairing ocular comfort.
- Demodex: a common parasite of both skin and eyelashes; associated with chronic blepharitis.
All these conditions reveal the indivisible link between eye and skin.
Analogy with the Periodontium: Lessons from Dentistry

The concept of Ophthalmoderma recalls the historical development of Dentistry with the Periodontium.
- Early 20th century: gum diseases were considered isolated problems.
- 1930–1950: the term periodontium was introduced to describe the complex of tissues (gums, ligament, bone, cementum).periodontium) για να περιγράψει το σύνολο ιστών (ούλα, σύνδεσμος, οστούν, τσιμέντο).
- 1960–1970: Periodontology was established as a new specialty.
- Today: no one refers to “gums” or “teeth” separately – the Periodontium is recognized as a unified ecosystem.
Similarly, Ophthalmology and Dermatology still treat eyes and skin separately. Dermophthalmology integrates them under one new scientific framework – the Ophthalmoderma.
Eyelids in Ophthalmology – From Peripheral to Central

Ophthalmology has always included eyelids in its scope:
- Conditions such as blepharitis, ectropion, entropion, trichiasis.
- Procedures such as blepharoplasty and trauma repair.
But eyelids are often approached individually, mainly as pathological or surgical problems, without emphasizing their role as part of the unified eye–skin ecosystem.
Dermophthalmology does not subtract from Ophthalmology – it enriches it:
- Places eyelids and eyelashes at the center of the Ophthalmoderma
- Links them with dermatological facial conditions,
- Highlights the need for daily preventive care, just as Periodontology did for oral health.
The Need for Multidimensional Eye Hygiene

Eye hygiene cannot be reduced to simple washing. Just as oral hygiene requires brushing, flossing, and mouthwash, Ophthalmoderma care must be multidimensional and daily:
- Eyelid and eyelash cleansing → removes sebum, debris, Demodex.
- Eyelid massage → improves microcirculation, reduces swelling and dark circles..
- Protective sprays → hydration, tear film stabilization, defense against irritants.
- Thermal therapy &meibomian gland evacuation → restores lipid layer balance,prevents dry eye and blepharitis,relieves eye fatigue, and improves visual quality even in healthy individuals as preventive care (Blackie et al., 2016).
Why Specialized Hygiene Products Are Needed

Simple water washing does not remove sebum, microbial biofilm, or Demodex from the eyelids.
Meanwhile, cleansing with soaps or shampoos is suboptimal::
- contain detergents that irritate the delicate periocular area,
- have a different pH from the ocular surface,
- may destabilize the tear film, causing dry eye, blurred vision, and irritation.
Even oil-based makeup removers, although effective at dissolving makeup, may leave residues that: make–up, μπορούν να αφήσουν υπολείμματα που:
- block meibomian glands,
- worsen gland dysfunction,
- και promote blepharitis and dry eye symptoms..
Dermophthalmology therefore recommends using specialized eyelid cleansers, such as foams formulated with:
- optimal concentrations of Tea Tree Oil (natural antibacterial & anti-Demodex activity),
- pH balanced for the ocular surface,
- mild yet effective composition for daily tolerance.

This ensures microbiome balance regulation, prevention of gland blockage, and preservation of tear film stability.
Dermophthalmology as a New Clinical Field

Dermophthalmology views Ophthalmoderma as a unified therapeutic target.
It is not enough to treat eye or skin separately; care must be comprehensive.
The World Organization of Dermophthalmology (WOD) promotes this vision globally, uniting Ophthalmologists and Dermatologists in a shared mission: improving health, beauty, and quality of life for the eyes.
Conclusion

Ophthalmoderma is not a theoretical construct – it is the reality of everyday clinical practice.
Just as the Periodontium was recognized as a new ecosystem and gave rise to Periodontology, Ophthalmoderma now leads to the birth of Dermophthalmology.
This new field enhances both Ophthalmology and Dermatology, offering a holistic framework for health, comfort, vision, and aesthetics.
For more practical eye care solutions, visit the Ophthalmogen range, the first in the world to apply the philosophy of Dermophthalmology.
References
- Lane SS, et al. A new system, the LipiFlow, for the treatment of meibomian gland dysfunction. Cornea. 2012.
- Blackie CA, et al. The sustained effect (12 months) of a single LipiFlow treatment for MGD and dry eye symptoms. Cornea. 2016.
- Matsumoto Y, et al. The evaluation of a warm moist air device for the treatment of dry eye syndrome. Cornea. 2006.
- Craig JP, et al. TFOS DEWS II Definition and Classification Report. Ocul Surf. 2017.