Introduction – The Paradox of Glaucoma
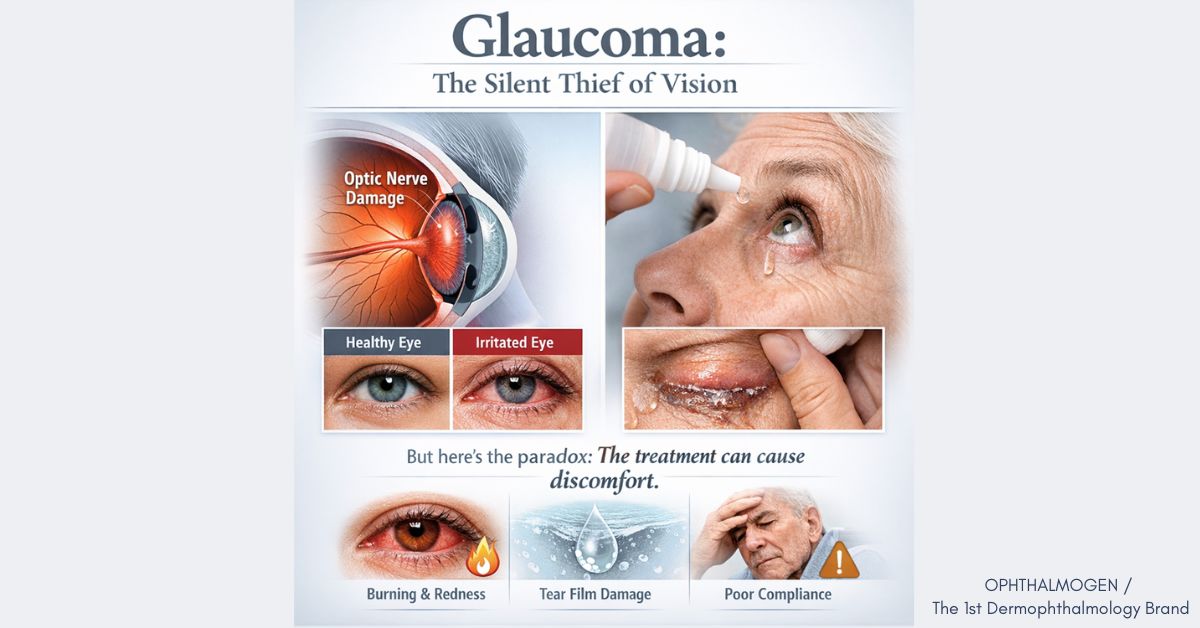
eyelid Glaucoma is the second leading cause of blindness worldwide, affecting over 70 million people. It is often called the “silent thief of sight” because it progresses without symptoms until it’s too late.
Treatment is based primarily on antiglaucoma eye drops that lower intraocular pressure and protect the optic nerve.
But here lies a paradox: τα ίδια τα φάρμακα που σώζουν την όραση συχνά προκαλούν σοβαρή ενόχληση στα μάτια.
The Side Effects of Glaucoma Drops
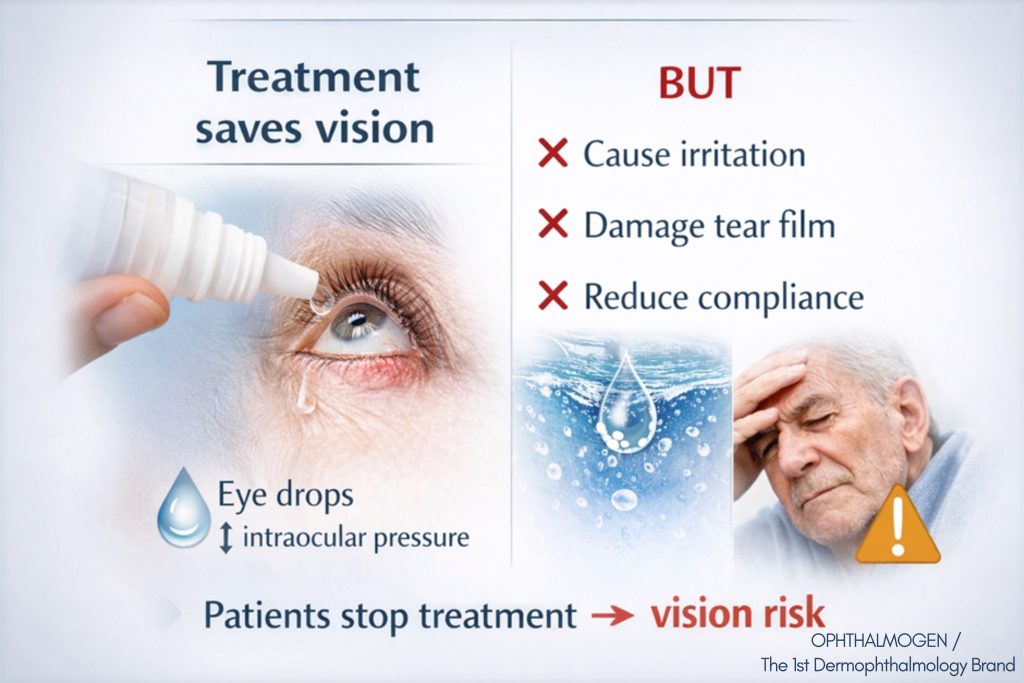
Many glaucoma patients report::
- red, tired eyes,
- tearing and burning,
- allergic reactions,
- dry eye and blurred vision.
Why?;
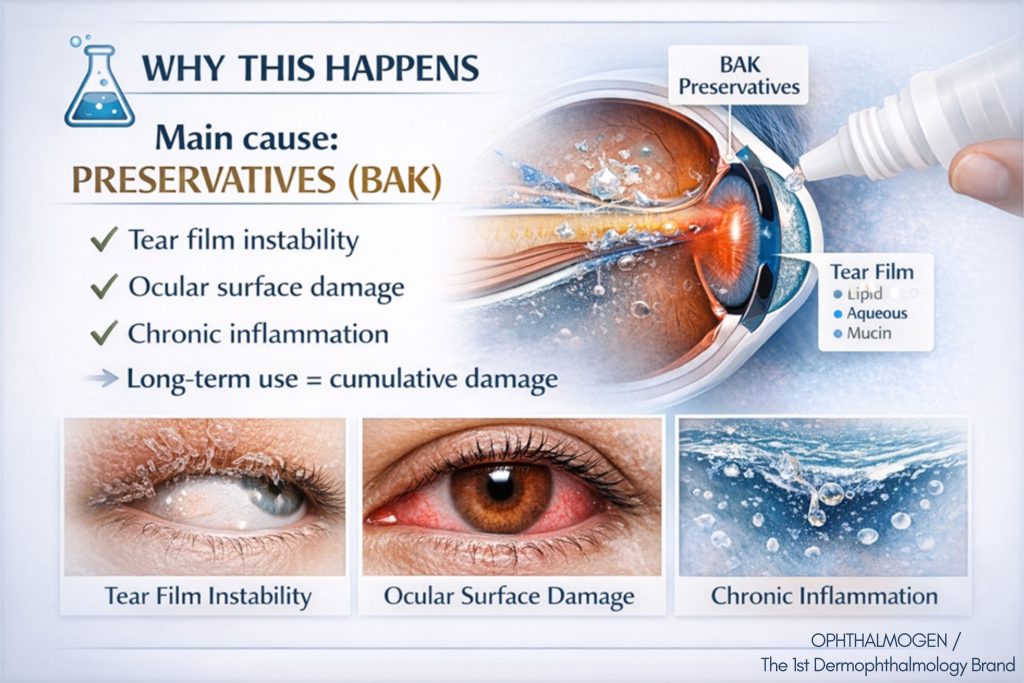
- Most drops contain preservatives (BAK – benzalkonium chloride) that damage the tear film and corneal epithelium.
- Long-term use (often 2–3 different drops per day for years or decades) leads to chronic inflammation and blepharitis.
- The result: patients often struggle with non-compliance, risking their sight.
Studies show that up to 30–40% of patients stop or skip their therapy within the first year due to side effects.

The Role of Eye Hygiene
This is where daily eyelid and ocular surface hygiene becomes essential.
Simple daily steps can::
- reduce inflammation,
- stabilize the tear film,
- relieve irritation,
- improve comfort,allowing patients to continue treatment.
Hygiene does not replace medication – it makes it more tolerable and effective.
Dermophthalmology in Glaucoma Care
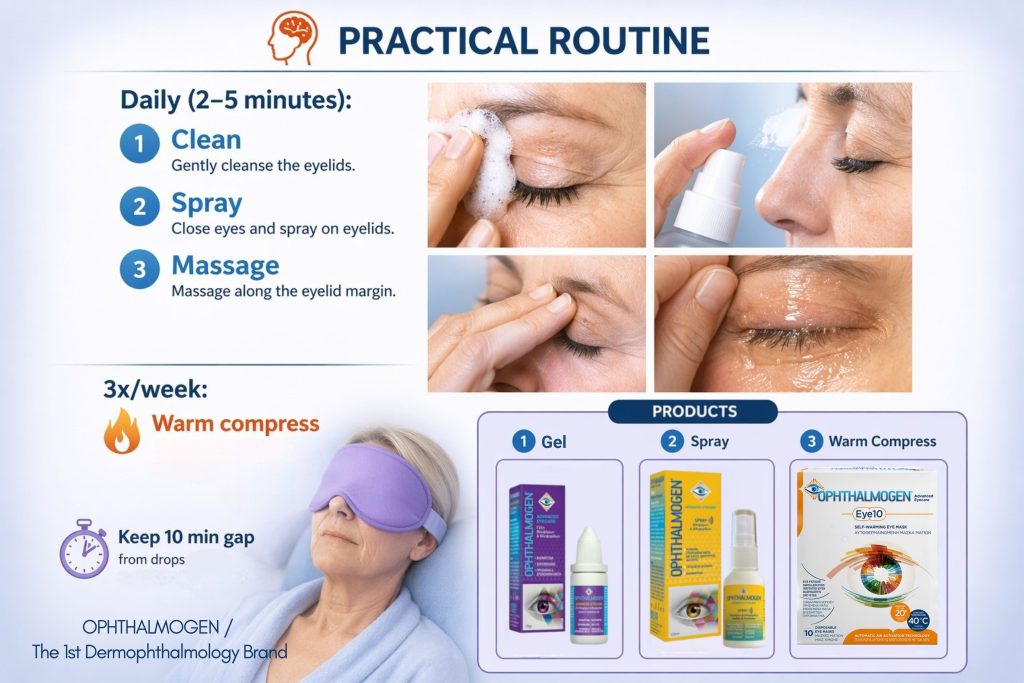
The new science of Dermophthalmology as promoted by the WOD – World Organization of Dermophthalmology provides practical tools that improve patient experience:
- Eyelid cleansing (Ophthalmogen&Naviblef): removes oil, makeup, toxic residues.
- Ophthalmogen Spray: controls microbial load &Demodex, balances the ocular microenvironment.
- Massage the eyelids at night with Ophthalmogen Gel: improves microcirculationreduces irritation, relaxes the eyelids.
- Ophthalmogen EYE10 thermotherapy: σταθερά 3 φορές την εβδομάδαunclogs meibomian glands, stabilizes tears.
For glaucoma patients, hygiene is not optional – it’s a partner to therapy.
The Human Dimension
Dry eye and irritation from glaucoma drops are not just “side effects.”For many patients, they are a source of frustration, anxiety, and social withdrawal.
Case study:
A 65-year-old patient with glaucoma frequently stopped using her drops because they “burned” her eyes. At the same time, she was terrified of going blind. With daily hygiene integrated into her routine, her symptoms decreased, and she was able to stick to therapy consistently.

Practical Guidelines for Glaucoma Patients
- Eyelid Cleansing: morning & evening with specialized products, not just water.
- Spray: 2–3 times per day to control the ocular microenvironment.
- Gel massage: το βράδυ, για ανακούφιση και καλύτερη αιμάτωση.
- Thermotherapy (EYE10): 3 φορές την εβδομάδα για αποσυμφόρηση αδένων.
- Χρονισμός: αφήστε 10 λεπτά απόσταση μεταξύ κολλυρίων και υγιεινής.
Conclusion
Glaucoma is not only about intraocular pressure. It is about the entire eye.
Daily eyelid and ocular surface hygiene:
- reduces symptoms,
- improves quality of life,
- increases compliance,
- enhances the effectiveness of therapy.
Dermophthalmology does not replace the ophthalmologist – it supports and empowers both doctor and patient.
FAQ
Q: Why are my eyes red and watery with glaucoma drops?
A: Most drops contain preservatives (e.g., BAK) that irritate the ocular surface. Hygiene reduces these symptoms.
Q: If I stop my drops because of discomfort, do I risk my vision?
A: Yes. Without treatment, the optic nerve is damaged. Instead of stopping, add daily hygiene to make drops more tolerable.
Q: Can hygiene replace my medication?
A: No. Hygiene does not replace glaucoma therapy, but it complements it, improving compliance and quality of life.
Q: Do all glaucoma patients need eye hygiene?
A: Yes – especially those using multiple drops or preserved formulations.